
About eight people have their heart stop unexpectedly every day in regional Victoria. Fewer than one in 10 survives.
Subscribe now for unlimited access.
or signup to continue reading
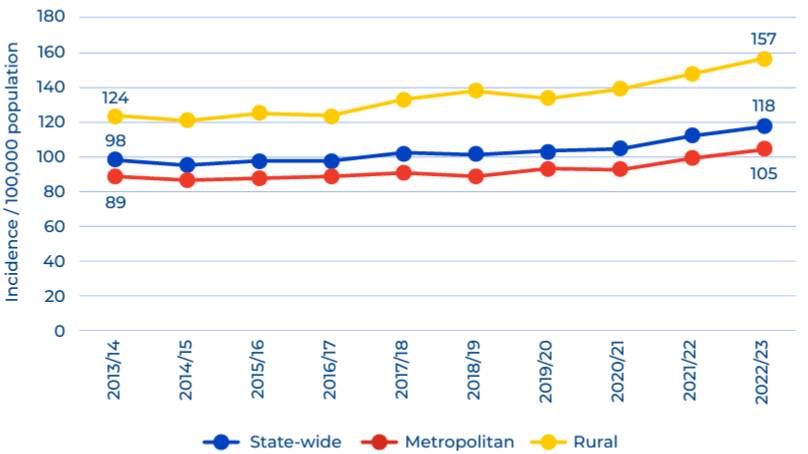
Cardiac arrests have hit an all-time high in country Victoria, with regional residents 50 per cent more likely to suffer an attack than Melburnians and more likely to die as a result, a report has shown.
The Victorian Ambulance Cardiac Arrest Registry (VACAR) released its 2022-23 stats on March 7, showing cardiac arrests had shot up across the state.
There were 7830 events across the state, nearly 2800 of them in regional areas, where the rate of cardiac arrest had risen by 15 per cent since the start of the COVID-19 pandemic.
You don't want to be alone
The VACAR report showed survival rates depended a lot on whether someone witnessed the cardiac arrest and provided lifesaving care.
One in eight patients who received bystander CPR survived the event, while just one in 20 survived if they had to wait for paramedics.
The rates were even better if a bystander had access to a defibrillator, with more than half of patients who received bystander defibrillation surviving.
But across Victoria only 30 per cent of cardiac arrests were witnessed by a bystander and the rate was even lower in regional areas. And even when the event was witnessed, bystanders only gave CPR 64 per cent of the time, with the rate again lower in the regions.
The map below shows cardiac arrest (OHCA) rates compared with bystander CPR (BCPR) rates across the state.
The purple and blue areas have high rates of bystander CPR, while the yellow, orange and red areas have low rates. Red areas are the deadliest, with high rates of cardiac arrest and low rates of bystander CPR.
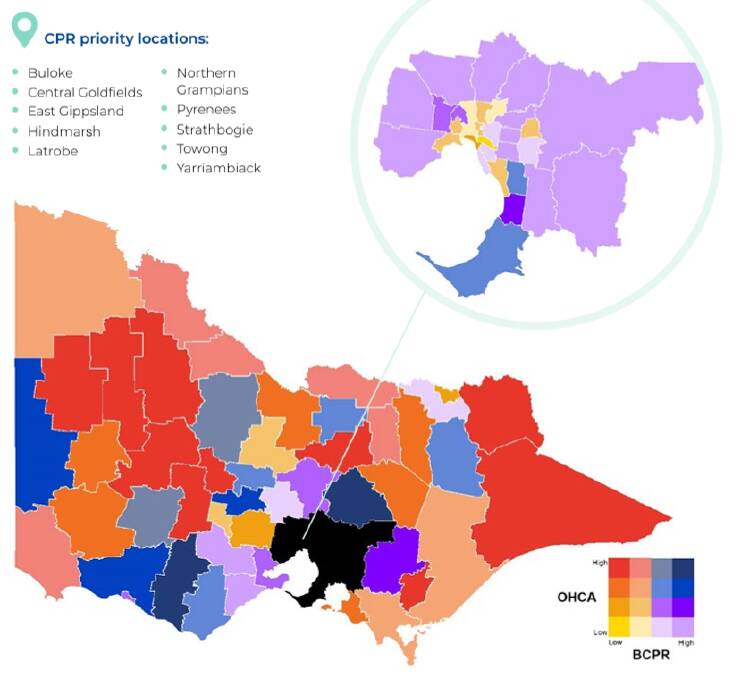
Some of the worst areas included the Central Goldfields, Northern Grampians and Pyrenees shires.
Grandmother saves her 'soulmate'
Portland grandmother Tuula Pratt proved the lifesaving value of bystander CPR when she resuscitated her husband of 36 years, Graham.
Mr Pratt had been reading in bed one morning in late 2023 when his heart suddenly stopped.
"Graham was making funny noises, and when I asked him if he was alright, he didn't answer," Ms Pratt said.
"When I looked into his eyes there was nothing, not even a flicker."
She called Triple Zero and during the call her husband stopped breathing.
"They told me an ambulance was on the way and to start CPR," Ms Pratt said.
She started chest compressions on Mr Pratt, made even harder by the fact he was lying on the couple's waterbed.
"It wasn't easy, but there was no way I could get him off of the bed," she said.

"It was exhausting but I just kept going, hoping they would get here in time."
Paramedics, firefighters and a GoodSAM Responder arrived minutes later and took over her husband's care.
Mr Pratt had lived with cardiomyopathy, a disease of the heart muscle, for many years, but there were no warning signs leading up to his cardiac arrest.
Portland paramedic Brittany Stafford said she didn't expect him to survive.
"It was a very complex case and he died at least three times while we were there," she said.
"After an hour working on him at home, we were finally about to transfer him to our helicopter, but he died again. It's the only time I've had to do CPR in a moving ambulance in my career."
Mr Pratt was finally stable enough to be flown to University Hospital Geelong, where he spent nine days in intensive care, and another two weeks in the cardiac ward.
He was fitted with an implantable defibrillator and was able to return home in January.
Ms Stafford said Ms Pratt's actions had made all the difference for her husband.
"So often these cases don't have a good outcome," she said.
"It just shows what a difference you can make in someone's survival, just by knowing CPR."


